As a Black woman and a mother of three, Kyara Banks can attest to not receiving quality and equal treatment during her pregnancy to her 10-year-old, 5-year-old, and 16-month-old baby.
“As black women, when we go in for our prenatal care, we are not really being heard at all,” she said. “Our concerns aren’t being taken seriously, and the postpartum care that we receive is more than inadequate. There is no reason why a mom who has just had a c-section should be waiting six weeks to have her first doctor’s appointment. That is entirely too long.”
In Ward 7 of Washington, D.C., the Healthy Babies Project aims to combat maternal mortality among black women by providing services to ensure safer births for at-risk pregnant women and their children.
“Once you’re at the point of delivering a baby, you’re at the end stage. Really, the whole basis of the Healthy Babies Project is to provide services to help mothers prepare for the baby prenatally. We want to help her from the moment she finds out that she is pregnant,” said youth service coordinator Jazmine Brazier.
For the past 27 years, HBP has built itself on being a non-formula driven center. It leads with the mission of wanting to assist at-risk families so that they may deliver healthy babies while transitioning from poverty into better life circumstances. HBP generally works with mothers and those who are expecting under the age of 24. It aims to reduce infant mortality, low birth weight rates, preventing unplanned pregnancies, providing prenatal parenting education and safe shelter.
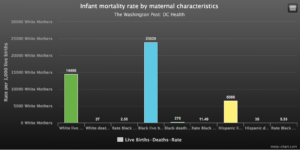
According to the Washington City Paper, in 2018 the District’s maternal mortality rate was 36.1 per 100,000 live births, while the national rate was 20.7. Black women in the District are three to four times more likely to die from childbirth than white women, and a leading cause of the high infant mortality rate is due to economic and social disparities that black mothers face every day. Instead of focusing on mortality rates, the Healthy Babies Project has started to combat these rates from the beginning of conception.
“I truly believe that when dealing with pregnancy, the health care system needs to care for black women more holistically. I should not be receiving the same treatment as a white woman,” Banks said. “Why? Because we don’t have the same history, we don’t have the same background or the same experiences. So whenever working with a black mom, they need to dig deeper because it’s more than just what’s on the surface.”
According to the Washington Post, half of the black women and more than 1 in 3 Hispanic women in D.C. are not entering prenatal care until their second or third trimester or not receiving care at all.
 “We’ve seen that women of childbearing age are the least likely to have gone to the doctor for a routine check-up, but each year their infants are still making their visits. What we find here is that mothers are taking their children to the doctor, but not themselves,” said Dr. Anjali Talwalkar, the deputy director of the Community Health Administration for the DC Department of Health.
“We’ve seen that women of childbearing age are the least likely to have gone to the doctor for a routine check-up, but each year their infants are still making their visits. What we find here is that mothers are taking their children to the doctor, but not themselves,” said Dr. Anjali Talwalkar, the deputy director of the Community Health Administration for the DC Department of Health.
“When I gave birth to my first child, I was 15 years old,” Banks said. ‘I did not get the attention or treatment that I needed, and I felt like I was not being heard. I was still a child having a child, and that care should have been a lot different. My oldest is 10 now, but really not much changed when I went in to have my youngest baby. The only difference was that I was actually able to go to a better hospital this time.”
After the closing of Providence and the United Medical Center’s maternity wards in Ward 7 and 8, the discussion has become whether black mothers in two of D.C.’s most impoverished communities were negatively impacted.
“They were not impacted as much as people have thought. Most mothers in Ward 7 and 8 were not even going to these facilities for many different reasons. But the closing of the medical centers definitely brought a lot of attention to the topic of infant mortality and maternal mortality in general,” said Talwalkar.
Linval Brown, HBP’s program director, agreed. “The closing of the Hospitals did not have that much of an impact on the women we work with, not a lot of people trusted them anyway,” he said. “They show a lot of disregard and disrespect for the women, so a lot of them were already going to other hospitals outside of their community where they are able to feel more human and receive better treatment. The fact that they are leaving doesn’t really bother anybody.”
Providence and United Medical Center did not respond to repeated requests for comment.
According to Dr. Talwalker, the leading cause of infant mortality primarily comes from the mother’s health before she became pregnant. She said, “Common causes of infant and maternal mortality for black women come from health issues already in the mother’s background. These are issues like heart problems, the obesity rate of black women, history of smoking, diabetes, and hypertension.”
“What we do here is the precursor to these young women having a baby. We educate these women on the advantage of taking care of themselves relative to having the baby. We want to make sure that the mentality that these young women enter with is not the same mentality that they leave with,” said executive director Regine Elie.
The Healthy Babies project empowers young mothers to take control of their own destiny. By keeping in contact with clients long after giving birth, this non-profit has aimed to emphasize and educate young mothers on the possibility of their dreams beyond motherhood.
Elie said, “An educated community is a more empowered community. While we definitely focus on medical care, our service goes beyond combating infant mortality. We truly feel as though it is more about the holistic approach of healing each woman of our community, one mother at a time.”



