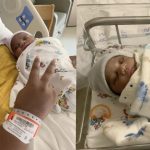
Breanna Bell, Howard University News Service
Washington, D.C.– Having a baby for some mothers in D.C.’s ward 7 and 8 can become overwhelming due to the complexity of the experience coupled with little to no immediate access to maternal care.
For some it may seem daunting. However, a small force of black doulas are working to make the process easier and giving those women access to the maternity care they need.
Jaime Baker, 35, a mother of two with another on the way, lives in ward 7. Along with the issues of searching for adequate prenatal and postpartum care, she says she’s experienced various difficulties when trying to receive proper medical assistance from hospitals. This is the reason why she’s used doulas for two of her children’s birthing journeys.
“You have a woman who understands you. You have an advocate for you and I felt like they didn’t care for me at Washington Hospitals,“ Baker said.
In D.C., black women are facing two major issues affecting childbirth. D.C. holds the highest maternal mortality rates in the country. According to an analysis of Centers for Disease Control and Prevention data, an average of about 39 women per 100,000 live births died in D.C. of causes related to pregnancies, from data sampled between 2005 and 2014.
The other major issue many women face when in search of a hospital or obstetrician is that of ‘hospital deserts’ in many parts of D.C. When Providence Hospital closed its maternity ward in 2017 as a cost saving measure, it left many low-income women with not many options outside the already scarce health choices.
Roughly around the same time, the city stopped deliveries to United Medical Center in Southeast because of many several mistakes, including failing to prevent an HIV infected mother from passing her disease to her infant, according to the Washington Post. When other transformations hit Medstar the same year, leaving many mothers planning on birthing their children in the hospital without many options, the east side of the nation’s capital was deemed a “maternity care desert.”
On average, paying for a doula’s work could range anywhere between $800 to $2500 by region. In the nation’s capital, doula services usually cost toward the farther end of the spectrum ($2000-$2500). There are many doula service providers in the district, but the options aren’t readily available for many women in the district.
Doulas are however, stepping up to fill the void in care.
Baker enrolled in the doula program at Mamatoto’s village in southeast D.C. not only because of the doulas trained in prenatal and postpartum care, but also because the organization works to grant access to their community at affordable pricing.
Charissa Young, one of D.C.’s community of doulas, has some experience in working with women affected by the lack of maternal care through her work with MamaToto’s Village, a perinatal family support organization in southeast D.C.
“They deal with that community of women who don’t have support,” Young said. “Their options are limited. Healthy options are limited. They might not have a car or access to healthy food options. There’s not many options and there’s not much choice. As a woman, that’s really debilitating.”
She continued, “It’s this amazing, magnificent, life changing thing we’re going through, but a lot of us are going through it alone in a way.”
For the most part, Young says her job is to offer that support and advocate for her clients as the liaison between midwives, doctors, and their patients, which is something that some women, especially first-time mothers, lack when they go without doulas.
“I think birth is 90% psychological. My whole job is to check in with your mindset. I do birth affirmations. Just to get you positively thinking about this. It’s going to be uncomfortable. Seeing and knowing that contractions come and go. My job is to get you as comfortable with it. Just having someone there for you and feeling comfortable and loved. Someone is there for you and you’re not alone.”
Traditionally, black women have had to help other women giving birth.
Muneera Fontaine, another practicing doula of 11 years, says it’s for a number of reasons. “Black women historically were looked at as breeders, but we weren’t necessarily feminine,” she said. “We were experimented on. It was believed that black women didn’t feel pain. That is something that has continued throughout the medical system. We’re ignored or we’re dismissed. We’re not given correct medical options.”
Maternal mortality has and continues to be an issue near to this doula’s heart. Fontaine claims she aims to change the narrative for many young and new mothers, and push the beauty of birth instead of the fear that’s been created in the uproar since news of maternal mortality rates in the US became popular.
“One of the things that has always bothered me is the narrative of fear. I’ve had girls tell me, ‘I’m scared to get pregnant. I’m afraid I’m going to die or my baby is going to die.’ Here and in the south, most midwives were black,” she said. “Many of them were poor but they served their community and black women had better statistics when they were cared for by their own.”
The creation of doulas can be traced all the way back to Greek civilization. The word “doula” in Greek translates to “female slave.” Before the civil war and the civil rights movement hit the south, black women were the primary caregiver of other black women giving birth. In the south, doulas were called “granny midwives.”
One simple trick that Fontaine says she continues to follow is to do her clients hair during delivery like the granny midwives in Louisiana who would carry a “fussin bag” so they could beautify a mother’s hair as she prepared for delivery.
One major issue to tackle in order to lower maternal mortality rates within the black community, is to begin having conversations about birthing with mothers, according to Fontaine. Both she and Young remembered not having very vivid conversations surrounding childbirth with their families. While Young was unsure as to the reasoning, Fontaine believes it’s due to a cycle which perpetuates trauma and dissociation from the birthing experience.
She cited a birthing practice called “twilight birthing,” which was popular in the 1930s through the 1960s. Doctors during this time would sedate mothers to render them unconscious in order to deliver babies. The problem with the practice was that many mothers weren’t entirely mentally unconscious so many would be forced to stay awake through delivery without having total control of their body.
“For many women, the traumatizing experience of this caused them to be silent about the whole birth,” Fontaine explained. “When mothers don’t talk about it, then their daughters learn not to talk about it.”
A major factor both Young and Fontaine noted that makes a difference for women giving birth is support and connection from medical providers during both pregnancy and postpartum.
According to Young, one point of contention many of her clients faced was the fact that they saw anywhere from three to five doctors and nurses with their obstetrician at the hospital; but, usually, it’s unknown who will be the doctor actually doing the delivery. With that, also comes uncertainty about adhering to the original birth plan.
“Hospitals, [doctors] probably have less time to deal with someone and the whole point is to get to know the mother. The whole thing is to just be a resource to her. They can’t give you that dedicated time,” she said. “A lot of people want someone to talk to.”
Baker said her first experience giving birth at a D.C. hospital, she felt unheard and her cries of pain were being ignored because of rigid protocols and a lack of attentiveness.
“When I went in, I was in pain. I wanted an epidural and that took a long time for me. I just felt like they were disregarding my pain levels,” she said. “I just slept for a while before I was monitored. When I first got there, it was just me and two other women, but it still took forever for me to be admitted. My mother had to basically advocate for me at that time.”
While Young and Baker see the lack of attention hospitals offer their expecting patients, Fontaine recognizes the lack of attention mothers receive after giving birth because most hospitals in the U.S. don’t offer any help for mothers postpartum. This, she claims, is another issue worth mentioning because traditionally, having a child brings communities together. In communities like the Amish and the Mennonites, it’s very common for people like neighbors or fellow church goers to offer to help to do things for the new family in order to make their lives easier.
“For the majority of mothers dying, these mothers die before or after childbirth. They’re not dying during birth. Birth and postpartum go together and we have to care for women on both sides,” said Fontaine.
For black women in D.C., some like Charissa Young believe that change has to start within the community of black women.
“We are not looked at as valued. And we also have to deem ourselves worthy of things,” Young said. “We as black women are getting there. I’m thinking about the underserved women. It’s our job as the older generation to let them know that they can do these things.
Knowledge is power. It requires us to really look into ourselves first. It’s not talked about as much in community settings but, the more we push for things, the more we can change. We have to change the culture for ourselves.”